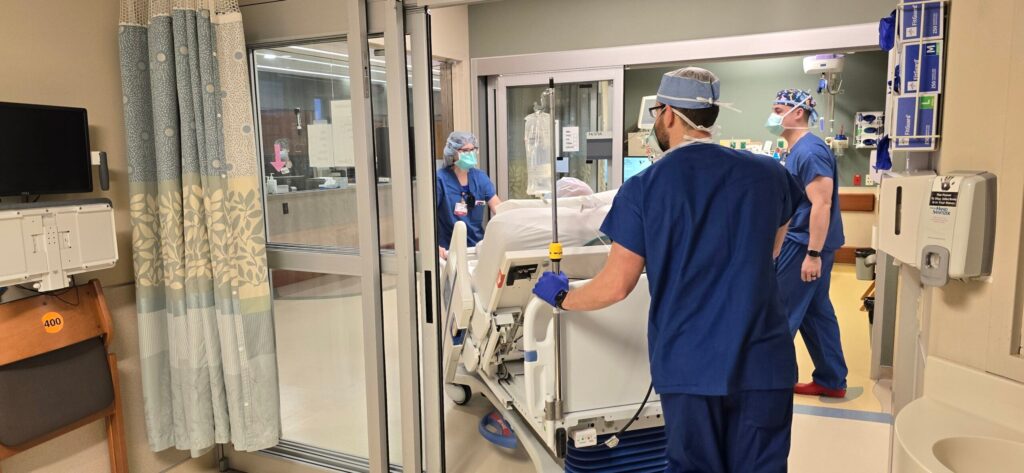
In the midst of fluctuating economic conditions, Wisconsin’s hospitals find themselves at a critical juncture. While financial stability showed signs of improvement last year, looming challenges such as rising operational costs and increasing numbers of uninsured individuals suggest that the road ahead may be rocky.
The Wisconsin Hospital Association (WHA) has unveiled its latest Guide to Wisconsin Hospitals, shedding light on the fiscal health of the state’s healthcare systems for 2024.
According to the report, operating margins for the 23 health systems, encompassing 129 hospitals, saw a modest recovery, rising from a negative 0.8 percent in 2023 to 2.2 percent in 2024. This uptick means that hospitals’ revenues slightly surpassed their expenses, yet this is just half of the margin seen pre-pandemic, as pointed out by Kyle O’Brien, president of the WHA.
O’Brien warned that the observed “modest improvement” might not persist, highlighting ongoing cost pressures, including those from government and commercial payers. Although the overall margins improved, some 60 hospitals recorded lower operating margins than in the previous year. Among them, 41 hospitals, including 17 critical safety net hospitals, operated at a loss.
Hospitals struggling financially often handle a larger share of patients on government insurance like Medicaid or Medicare, which typically reimburse less than the cost of care, according to O’Brien. Additionally, reimbursement challenges with commercial insurers and Medicare Advantage plans are becoming more pronounced, affecting hospital operations.
“You’re seeing that in a lot of areas throughout the state, where hospitals are saying, ‘No, we can’t agree to a contract any longer because the rates that were being provided aren’t sufficient to actually keep up with the cost of delivering care to patients,’” O’Brien remarked, noting changes in the marketplace over the past decade.
The financial squeeze is further exacerbated by rising expenses. The report indicates that since 2022, costs for supplies and services have surged by 11 percent, while salaries and fringe benefits have risen by 10 percent, driven by an ongoing workforce shortage.
O’Brien emphasized that the cost increases in medical devices and pharmaceuticals are significant contributors to hospitals’ financial burdens.
Adding to the uncertainty, potential federal cuts to Medicaid and Affordable Care Act (ACA) subsidies threaten to increase the number of uninsured individuals. Work requirements for Medicaid recipients, slated for 2027 implementation, could exacerbate this issue. The KFF notes that while these requirements may not boost employment, they are expected to elevate uninsured rates.
Similarly, the withdrawal of enhanced ACA subsidies could lead to a projected 26 percent hike in marketplace premiums, as reported by KFF. Stuart Craig, an associate professor at the University of Wisconsin-Madison, explained that making ACA plans less affordable could deter enrollment, underscoring hospitals’ preference for insured patients.
“Lots of hospitals will have a cash price that they offer when they know you don’t have insurance that’s maybe lower than what they would charge somebody in another situation,” Craig said. “But in most situations, they would prefer that person to be covered.”
To mitigate these potential issues, the WHA advocates for maintaining the enhanced ACA subsidies. O’Brien noted that if Medicaid work requirements transition individuals to commercial insurance, it could be beneficial for hospitals, though the association remains wary of potential coverage losses in 2027.
“Hospitals are always concerned if there is the potential that somebody loses coverage because hospitals are the one provider that has to serve everybody, regardless of their ability to pay,” O’Brien stated.