In the rural landscape of Northcentral Pennsylvania, Dr. Ethan Gable undertakes a significant commute, traveling 40 miles between two hospitals where he serves as an obstetrician and gynecologist. His journey highlights a broader issue: the decline of obstetric services in rural areas.
Dr. Gable is one of three OB/GYNs at UPMC Wellsboro in Tioga County and UPMC Cole in Potter County. His dedication is part of a strategic effort to maintain crucial medical services for rural communities. “Absolutely, it’s a priority,” stated Patti Jackson, UPMC North Central PA market president, emphasizing the necessity of innovative solutions to overcome challenges.
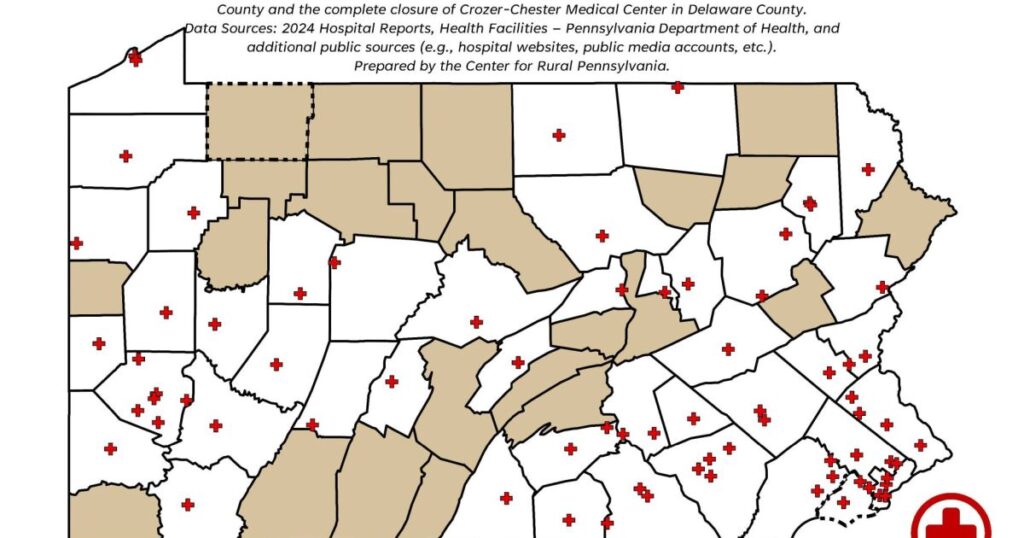
In Pennsylvania, finding obstetric care in rural counties is increasingly difficult. The Center for Rural Pennsylvania notes that 23 out of 67 counties lack hospitals offering labor and delivery services, and all of these are rural.
The Shrinking Presence of Obstetric Units
According to the Chartis Center for Rural Health, Pennsylvania has seen a 42% reduction in rural obstetric units from 2011 to 2024, ranking third nationally in this decline.
Michael Topchik, the executive director, explained, “When we ask CEOs why, it’s very expensive, it’s very risky and increasingly difficult to provide the high level of service and technology and everything else that’s needed to go along with that care.”
Topchik warns that the reduction in specialized services often signals broader financial issues for rural hospitals. “We haven’t seen a statistical correlation, but we do see alignment directionally. I use the term bellwether, it’s a canary in a coal mine, so to speak,” he said.
Dr. Gable pointed out another challenge: declining birth rates, which affect the clinical capacity to maintain service levels. With UPMC Cole ceasing labor and delivery services in April, rural healthcare’s adaptability is tested. Patients are now directed to UPMC Wellsboro, where Gable continues his commitment to maternal and infant health.

Dr. Gable leverages technology for patient care. “Say it’s a Cole patient, she can physically go into our office, she sees the nurse… and then she actually remotes in to see me at another hospital,” he explained, describing efforts to bring medical care closer to patients.
Expanding Maternity Care Deserts in Pennsylvania
The closure of Warren General Hospital’s labor and delivery unit adds to the state’s growing maternity care desert, affecting an eight-county region with 35,000 women of childbearing age. This area is now without local labor and delivery services, a region larger than Connecticut, according to Zachary Adams of the Center for Rural Pennsylvania.
Residents of these counties face significant travel distances to receive care. For example, someone in Susquehanna County must travel about 42 miles to the nearest hospital offering labor and delivery services.
“You could imagine a scenario where those doctors in the remaining labor and delivery units are seeing an increase in their patient load… we might expect to see an increase in emergency department cases,” said Zachary Adams.
Impact on Rural Areas
Rural areas face a stark shortage of OB/GYNs compared to urban regions. Kaitlyn Goode from the Center for Rural Pennsylvania noted that rural areas have 6 OB/GYNs per 100,000 population, whereas urban areas have 16.

Topchik warns of potential exacerbation due to Medicaid cuts, which could disproportionately impact rural healthcare. With Medicaid covering many births, such reductions could significantly affect rural hospitals’ financial health.
KFF Health News estimates federal Medicaid spending cuts will increase the number of uninsured Americans by 7.5 million over the next decade, with a $5.5 billion reduction in Pennsylvania alone.
Addressing Women’s Health Shortages
UPMC is combating these challenges with telemedicine and a new residency model for rural obstetric care. “We have telemedicine set up so that a patient can… set up an appointment with me,” Gable said, describing flexible options for patient care.
Patti Jackson elaborated on UPMC’s residency model, highlighting the integration of family medicine residents into women’s health teams to bolster care capabilities.
Topchik sees potential in the Rural Health Transformation Program, which allocates $50 billion to states over five years. Pennsylvania received $193 million this year, with a focus on maternal health improvements.