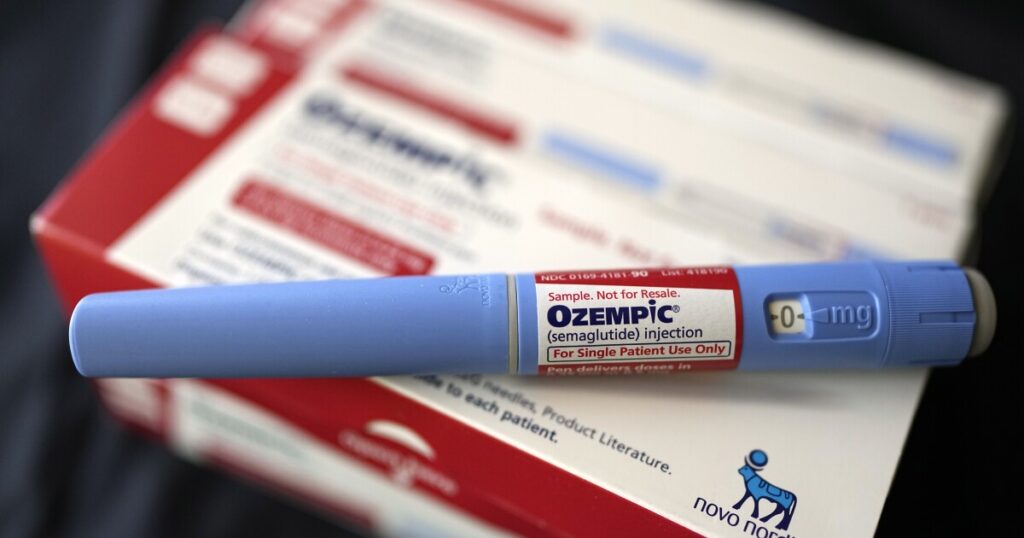
In a significant policy shift, Pennsylvania will restrict access to certain weight-loss medications for Medicaid recipients starting January. While drugs like Ozempic and Wegovy will no longer be funded for obesity alone, they will still be available for diabetes treatment and other medical conditions.
This decision is part of an initiative to curb the rising expenses associated with GLP-1 receptor agonists, medications known for their hefty price tags. The state aims to alleviate the financial burden on its Medicaid system, which is anticipated to spend over $1.3 billion on these drugs this year, as outlined in a plan introduced by Gov. Josh Shapiro’s administration (source).
The change has stirred debate among lawmakers who previously discussed the medication costs during budget hearings (source). McCandless state Rep. Arvind Venkat, an emergency physician, expressed concern, stating, “To simply restrict coverage is penny-wise and pound-foolish.” He emphasized the preventive health benefits these medications offer, particularly for heart and kidney diseases.
Venkat reported that recipients have been informed of the impending coverage change, though the communication lacks clarity. “If DHS is restricting access, they owe it to the public to explain what their rationale is,” Venkat remarked.
Obscure Notifications Sent to Patients
A letter reviewed by WESA reveals that medications containing GLP-1 receptor agonists will not be covered unless linked to a qualifying condition. The letter, however, fails to explain the reasons behind the decision, leaving recipients with the option to appeal before the year’s end.
According to a Department of Human Services (DHS) spokesperson, affected Medicaid recipients will receive detailed notices this month, explaining the changes and how to appeal them. The announcement was discreetly made via a DHS bulletin last week, sent by state Medicaid director Sally Kozak to healthcare providers (source).
The price and utilization of GLP-1s have been cited as unsustainable, with costs escalating from $223.3 million in 2022 to $650 million over two years, and reaching over $1.3 billion in 2025. This information was documented in minutes from an April meeting of the Pharmacy and Therapeutics committee.
Other states, including Wisconsin and Rhode Island, are also contemplating similar restrictions (source). As of October, 16 states offered GLP-1 coverage for obesity, with several states covering the drugs for other uses except obesity alone (source).
‘A Step in the Right Direction’
Some Pennsylvania politicians support the decision. State Sen. Scott Martin (R-Lancaster), who chairs the Appropriations Committee, described the reform as “a step in the right direction.” He emphasized the importance of scrutinizing GLP-1 prescriptions within taxpayer-funded programs like Medicaid.
Meanwhile, Squirrel Hill state Rep. Dan Frankel acknowledged the drug’s benefits but noted its financial implications. He highlighted the budgetary challenges posed by federal mandates, suggesting limited state resources to bridge funding gaps.
Efforts to regulate prescription costs have gained little traction. Venkat has advocated for a bipartisan bill to reduce GLP-1 costs through a subscription model, which remains pending in the House Human Services committee (source).
Patients who mistakenly receive notifications about the benefit change may appeal, as advised by Kyle Fisher of the Pennsylvania Health Law Project. He noted that individuals under 21 and those with specific health conditions could still qualify for the medication.
Read more from our partners at WESA.